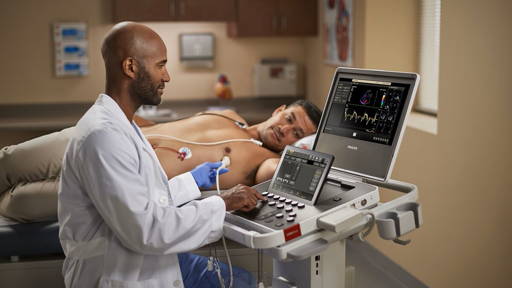
In one demonstration, Sarah Murthi, MD, associate professor at the University of Maryland School of Medicine (UMSOM) and trauma surgeon at the R Adams Cowley Shock Trauma Center, let visitors experience how an ultrasound examination looks with the addition of augmented reality. With the help of volunteer “patient” Eric Lee (research programmer at the UM Institute for Advanced Computer Studies in College Park), Murthi demonstrated visualization headgear. Using the headgear, doctors can keep their eyes on the patient while seeing images of the ultrasound – and potentially much more information added to their view.
According to Murthi, ultimately, the whole medical staff might be wearing these masks. Then, whoever wants to, can see the imaging. Keeping all of the critical information about a patient in plain view might also help avoid problems doctors currently encounter, such as missing changes in vital signs while focusing on an ultrasound scan. “The other real thing that happens is that you’ll be all caught up in the imaging and meanwhile the patient’s blood pressure drops and they become unstable.” ###VR###
Both Murthi and Hong stressed the great educational value of virtual and augmented reality. “Once this virtual world is created and it can rebroadcast in real time, a thousand people could watch at the same time and learn whatever lesson they needed to learn,” said Murthi.
Other medical uses for virtual reality around the country were discussed during the March 27 meeting, including the use of three-dimensional mapping to plan and practice brain surgery, developing clinically guided scenarios for soldiers experiencing Post Traumatic Stress Disorder, and reducing the experience of pain during burn treatments by engaging patients in interactive virtual reality games.
“Our focus has been to look for technologies that we could have in hospitals soon, in the next year or so since a lot of this equipment already exists,” said Murthi. “The question is how can we use it and develop it so we can already start saving lives.”
According to Murthi, ultimately, the whole medical staff might be wearing these masks. Then, whoever wants to, can see the imaging. Keeping all of the critical information about a patient in plain view might also help avoid problems doctors currently encounter, such as missing changes in vital signs while focusing on an ultrasound scan. “The other real thing that happens is that you’ll be all caught up in the imaging and meanwhile the patient’s blood pressure drops and they become unstable.” ###VR###
Virtual reality
In another demonstration, Caron Hong, MD, associate professor at UMSOM and a critical care anesthesiologist at Shock Trauma, helped visitors use virtual reality goggles to place an endotracheal tube through the mouth of a medical mannequin and into its airway. Intubation is a common procedure, used when a patient needs assistance breathing, that requires considerable practice to master.Both Murthi and Hong stressed the great educational value of virtual and augmented reality. “Once this virtual world is created and it can rebroadcast in real time, a thousand people could watch at the same time and learn whatever lesson they needed to learn,” said Murthi.
Combining VR, AR
She added that a combination of virtual and augmented reality may one day support the care of battlefield patients. First responders on the ground might use augmented reality to see important data and imaging while treating and transporting patients. At the same time, advanced medial staff at a remote location could use virtual reality to see what first responders are seeing and provide valuable insight and information to first responders.Other medical uses for virtual reality around the country were discussed during the March 27 meeting, including the use of three-dimensional mapping to plan and practice brain surgery, developing clinically guided scenarios for soldiers experiencing Post Traumatic Stress Disorder, and reducing the experience of pain during burn treatments by engaging patients in interactive virtual reality games.
“Our focus has been to look for technologies that we could have in hospitals soon, in the next year or so since a lot of this equipment already exists,” said Murthi. “The question is how can we use it and develop it so we can already start saving lives.”