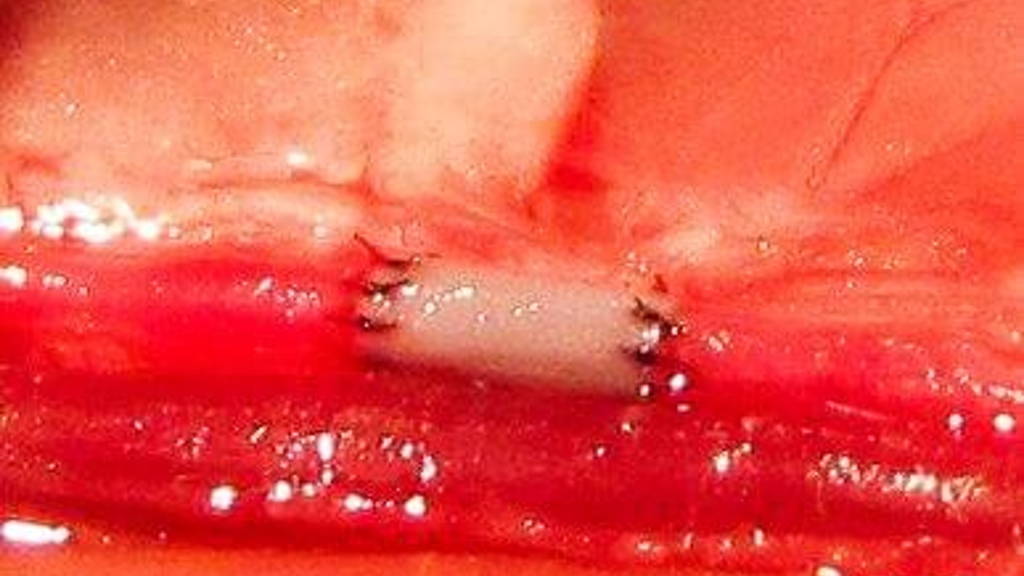
The new bioengineered blood vessels are the smallest yet that are also strong enough to be used in parts of the body where exceptionally tiny blood vessels are needed, such as the fingers. The technique has succesfully been tested on rats and was reported online in January in the journal Tissue Engineering. The research was funded by the National Institute of Biomedical Imaging and Bioengineering (NIBIB).
“The ability to link an engineered tissue to a patient’s circulatory system is as important as creating the implant itself,” says Rosemarie Hunziker, Ph.D., director of the NIBIB program in Tissue Engineering. “This study is key because they have developed a “linker” that has properties compatible with natural human blood vessels and is also easy to manipulate. It is an important accomplishment.”
In addition, the research focuses on connecting very small arteries, which is particularly difficult and is needed for attaching artificial implants as well as delicate replantation surgeries where a patient’s damaged tissue must be reconnected or repaired. Tissue damage from traumatic injuries often leaves many small stubs of blood vessels that need a linking segment to successfully reconnect the tissue to the vasculature.
The new technique is able to produce grafts with diameters smaller than previously possible, allowinging connection to tiny arteries in the body, like in the fingers. “If you needed some sort of bridge to connect the circulation of a severed finger to the intact circulation of the patient then you need to be able to create grafts at around the one millimeter scale,” says Joe Tien, Ph.D., professor of biomedical engineering at Boston University and senior author of the paper. “And there’s not really much known about trying to create an artificial graft that small.”
Tien’s group discovered that drying a large piece of collagen on a small, rotating rod, “like a rotisserie for a chicken,” says Tien, makes it shrink down to the very small diameter of the rod, becoming more dense in the process. The resulting structure can then be crosslinked, adding the critical additional strength.
The combination of drying and crosslinking was the key to the team’s success. When they implanted the collagen tubes in rats, they were able to attach them to the rat’s circulation and demonstrate that the tubes sustained normal blood flow for twenty minutes and displayed strengths similar to an artery in a rat’s leg.
The researchers already demonstrated the ability to line the tubes with endothelial cells, which grow well on the collagen. The next test is to see how the system responds to lined tubes long term and if these artificial vessels display irregularities, degrade, or fail for any reason.
“The ability to link an engineered tissue to a patient’s circulatory system is as important as creating the implant itself,” says Rosemarie Hunziker, Ph.D., director of the NIBIB program in Tissue Engineering. “This study is key because they have developed a “linker” that has properties compatible with natural human blood vessels and is also easy to manipulate. It is an important accomplishment.”
Collagen tubes
The Boston University team developed a method that uses collagen tubes to make the critical connections. They demonstrated that their collagen constructs were compatible with a rat’s vascular system and connected seamlessly, without leaking or causing blockage.In addition, the research focuses on connecting very small arteries, which is particularly difficult and is needed for attaching artificial implants as well as delicate replantation surgeries where a patient’s damaged tissue must be reconnected or repaired. Tissue damage from traumatic injuries often leaves many small stubs of blood vessels that need a linking segment to successfully reconnect the tissue to the vasculature.
The new technique is able to produce grafts with diameters smaller than previously possible, allowinging connection to tiny arteries in the body, like in the fingers. “If you needed some sort of bridge to connect the circulation of a severed finger to the intact circulation of the patient then you need to be able to create grafts at around the one millimeter scale,” says Joe Tien, Ph.D., professor of biomedical engineering at Boston University and senior author of the paper. “And there’s not really much known about trying to create an artificial graft that small.”
Easy way of grafting
Using collagen, Tien and his team discovered an easy way to make such a graft; by drying. Collagen is a natural substance found in the body, so it’s compatible, and cells are able to adhere and grow on it with less risk of an adverse reaction compared to synthetic materials. But because collagen is normally very dilute — it’s 99 percent water — a common technique that binds proteins to each other to add stability and strength, known as crosslinking, didn’t work: there weren’t enough solid materials to connect.Tien’s group discovered that drying a large piece of collagen on a small, rotating rod, “like a rotisserie for a chicken,” says Tien, makes it shrink down to the very small diameter of the rod, becoming more dense in the process. The resulting structure can then be crosslinked, adding the critical additional strength.
The combination of drying and crosslinking was the key to the team’s success. When they implanted the collagen tubes in rats, they were able to attach them to the rat’s circulation and demonstrate that the tubes sustained normal blood flow for twenty minutes and displayed strengths similar to an artery in a rat’s leg.
Extending unobstructed blood flow
Next, the team hopes to extend the time the grafts can maintain unobstructed blood flow. Bare, empty tubes are likely to lead to blood clot formation, but tubes lined with endothelial cells, which naturally line blood vessels, reduce the risk of clotting.The researchers already demonstrated the ability to line the tubes with endothelial cells, which grow well on the collagen. The next test is to see how the system responds to lined tubes long term and if these artificial vessels display irregularities, degrade, or fail for any reason.