Digital health solutions promise to change the way healthcare is provided, driving progress toward universal health coverage and transforming outcomes for patients with NCDs.
Worldwide, non-communicable diseases (NCDs) are responsible for more deaths than any other disease
Non-communicable diseases account for approximately 70% of deaths worldwide, of which three-quarters occur in low- and middle-income countries (LMICs).1 Funding for tackling NCDs is low compared to other diseases and preventive measures in particular would have a significant impact.
To combat NCDs, we need to transform the way healthcare is provided and expand access to all. Without properly addressing NCDs, universal health coverage (UHC), a target of Sustainable Development Goal (SDG) 3, cannot be achieved
Health systems must move toward universal health coverage and shift…
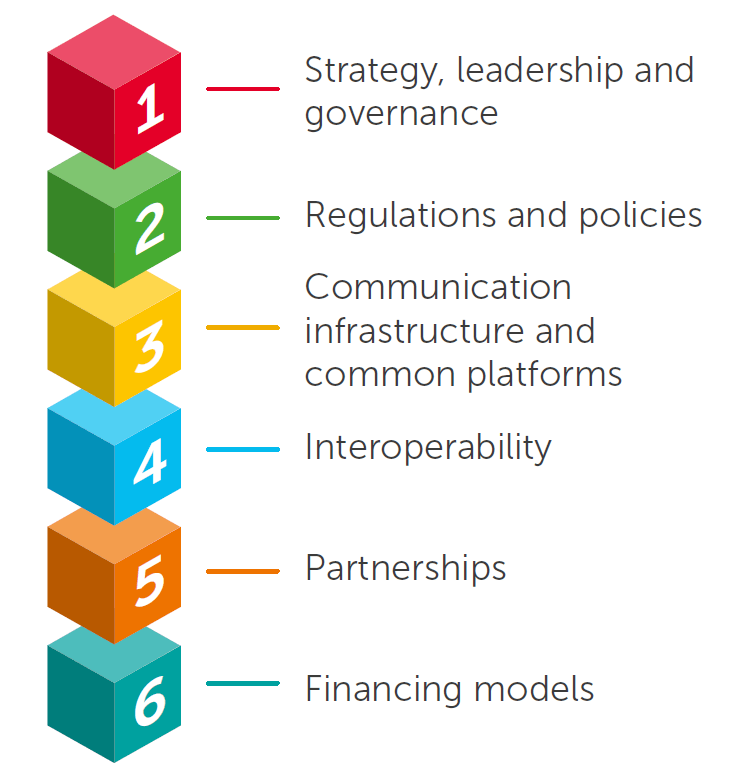 Building Blocks for Sustainable Digital Health. There is much policymakers can do to create favorable environments for sustainable digital health, and they don’t have to do it alone. Six building blocks can help countries realize the promise of digital health and transform access to appropriate, effective NCD care.[/caption]
To maximize the impact of digital health on NCDs in order to accelerate the achievement of UHC, solutions have to be financially sustainable
Many digital health solutions are launched as pilots and are often not designed for scale and sustainability. This can lead to a fragmented, uncoordinated landscape of standalone initiatives. The simplest solutions – namely those designed with the needs of the end user in mind, that use existing technologies and are integrated in the existing health system, and which are widely available in the context – have the highest chances of being scalable and sustainable. This is demonstrated, for example, by the national scaling of telemedicine services in Ghana.
The report provides examples, insights and recommendations for greater sustainability in digital health. Download the full report here.
Building Blocks for Sustainable Digital Health. There is much policymakers can do to create favorable environments for sustainable digital health, and they don’t have to do it alone. Six building blocks can help countries realize the promise of digital health and transform access to appropriate, effective NCD care.[/caption]
To maximize the impact of digital health on NCDs in order to accelerate the achievement of UHC, solutions have to be financially sustainable
Many digital health solutions are launched as pilots and are often not designed for scale and sustainability. This can lead to a fragmented, uncoordinated landscape of standalone initiatives. The simplest solutions – namely those designed with the needs of the end user in mind, that use existing technologies and are integrated in the existing health system, and which are widely available in the context – have the highest chances of being scalable and sustainable. This is demonstrated, for example, by the national scaling of telemedicine services in Ghana.
The report provides examples, insights and recommendations for greater sustainability in digital health. Download the full report here.
- from facility-based care to community-based care with a focus on increasing health system capacity and efficiency
- from episodic, curative care to long-term, continuous care to institute a people-centered focus with improved access
- from reactive care to proactive, preventive care featuring forward-looking health management with improved transparency
The myriad of digital health solutions often lack a clear strategy and purposeInvesting in digital health to strengthen entire health systems can accelerate efforts to combat NCDs, and by the same token, investing in digital health specifically to combat NCDs can have wider health system benefits. Ultimately, digital health is a catalyst in transforming how healthcare is delivered and experienced, as it allows LMICs to move from disease silos in healthcare to an integrated, resilient health system. Digital technology is driving innovation in healthcare, especially in LMICs Unmet health needs driven by a lack of health infrastructure and trained health workers, widespread mobile penetration and relatively open regulatory environments make LMICs fertile ground for innovation. And with fewer entrenched, legacy systems to overcome, countries have an opportunity to “leapfrog” and adopt newer solutions faster. Digital health should be considered an essential part of the healthcare system, just as medical equipment or hospital beds are. The results so far are encouraging A few studies have evaluated the impacts of digital health, ranging from patient-level results like reduced blood glucose levels to system-level results such as improved access to services and cost savings. In Canada, for example, the cumulative benefits of investing in digital health were estimated at around CAD$16 billion over the course of nine years. The results so far are encouraging and could be used to drive further investment and scaling of digital health solutions. [caption id="attachment_25521" align="alignright" width="736"]
 Building Blocks for Sustainable Digital Health. There is much policymakers can do to create favorable environments for sustainable digital health, and they don’t have to do it alone. Six building blocks can help countries realize the promise of digital health and transform access to appropriate, effective NCD care.[/caption]
To maximize the impact of digital health on NCDs in order to accelerate the achievement of UHC, solutions have to be financially sustainable
Many digital health solutions are launched as pilots and are often not designed for scale and sustainability. This can lead to a fragmented, uncoordinated landscape of standalone initiatives. The simplest solutions – namely those designed with the needs of the end user in mind, that use existing technologies and are integrated in the existing health system, and which are widely available in the context – have the highest chances of being scalable and sustainable. This is demonstrated, for example, by the national scaling of telemedicine services in Ghana.
The report provides examples, insights and recommendations for greater sustainability in digital health. Download the full report here.
Building Blocks for Sustainable Digital Health. There is much policymakers can do to create favorable environments for sustainable digital health, and they don’t have to do it alone. Six building blocks can help countries realize the promise of digital health and transform access to appropriate, effective NCD care.[/caption]
To maximize the impact of digital health on NCDs in order to accelerate the achievement of UHC, solutions have to be financially sustainable
Many digital health solutions are launched as pilots and are often not designed for scale and sustainability. This can lead to a fragmented, uncoordinated landscape of standalone initiatives. The simplest solutions – namely those designed with the needs of the end user in mind, that use existing technologies and are integrated in the existing health system, and which are widely available in the context – have the highest chances of being scalable and sustainable. This is demonstrated, for example, by the national scaling of telemedicine services in Ghana.
The report provides examples, insights and recommendations for greater sustainability in digital health. Download the full report here.