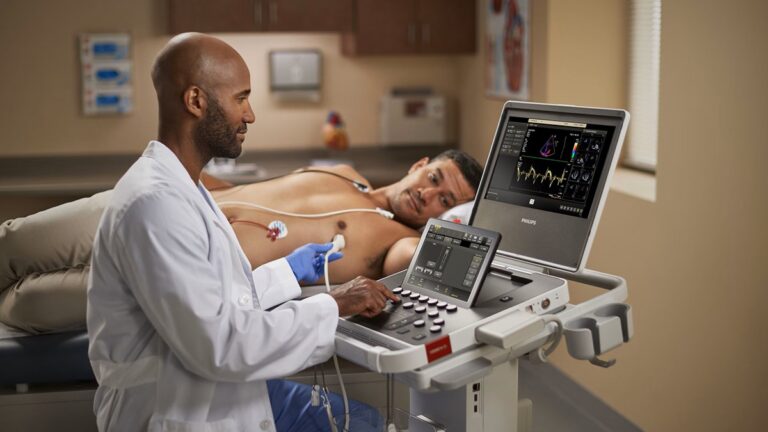
The key to the technology is a fingernail-sized microchip that mounts onto a traditional ultrasound probe — the plastic scanner that slides over gel-slathered skin to relay two-dimensional images of what lies beneath. This way, technology that keeps track of how a smartphone is oriented can give $50,000 ultrasound machines many of the 3-D imaging abilities of their $250,000 counterparts — for the cost of a $10 microchip.
Stitching 2D slices into 3D image
The chip registers the probe’s orientation, then uses software to seamlessly stitch hundreds of individual slices of the anatomy together in three dimensions. This result in an instant 3-D model similar in quality to a CT scan or MRI, according Joshua Broder, M.D. The emergency physician and associate professor of surgery at Duke Health is one of the creators of the technology.
Two-D ultrasound machines with higher resolution have clearer 3-D pictures, Broder says. “With 2-D technology you see a visual slice of an organ, but without any context, you can make mistakes. These problems can be solved with the added orientation and holistic context of 3-D technology. Gaining that ability at an incredibly low cost by taking existing machines and upgrading them seemed like the best solution to us.”
Broder first worked on his own for a year and then took sketches to Duke’s Pratt School of Engineering. There he connected with then-undergraduate Matt Morgan, and biomedical engineering instructors and professors Carl Herickhoff and Jeremy Dahl, who have since taken positions at Stanford where they continue to develop the device.
Check out this video for an example of how the technology works:
###Ultrasound-chip###
3D printing for prototypes
The team has used Duke’s own 3-D printing labs to create their prototypes, which start with a streamlined plastic holster that slips onto the ultrasound probe. A technician can use the probe as usual, or add 3-D images by simply snapping on a plastic attachment containing the location-sensing microchip.
To get the best 3-D images, the team also devised a plastic stand to help steady the probe as the user hones in on one part of the anatomy. The microchip and the ultrasound probe connect via computer cables to a laptop programmed for the device. As the user scans, the computer program creates a 3-D model in seconds.
Fitting technology in flow patient care
Both Duke and Stanford are testing the technology in clinical trials to determine how it fits in the flow of patient care. The creators believe some of the most promising uses could be when CT scans or MRIs are not available, in rural or developing areas, or when they are too risky – for example when you don’t know if a trauma patients condition will worsen when moved to a CT scanner.
Broder: “With our new 3-D technique, we hope to demonstrate that we can determine the source of bleeding, measure the rate of bleeding right at the bedside and determine whether an operation is really needed.”
Newborn babies are also notoriously difficult to get images of, but doctors may need numerous scans when babies are born with fluid on the brain or a congenital condition. MRI machines require patients to be still for minutes at a time, which often means sedating an infant. CT scans provide excellent 3-D images, but expose the infant to radiation.
The team is now working to bridge some of gaps between their adapted 3-D ultrasound and 3-D machines already on the market, such as the ability to capture a beating heart in motion.